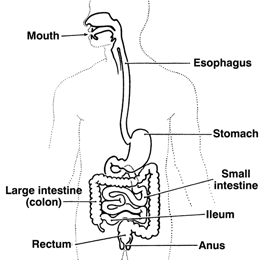
Pseudo-Obstruction:
Intestinal pseudo-obstruction is a uncommon disorder characterized by symptoms resembling those of a bowel obstruction or intestinal blockage.
These symptoms result from issues with nerves or muscles, disrupting the normal movement of food, fluid, and air through the intestines.
While this condition can affect individuals of any age, it is more frequently observed in children and older adults.
In children, there is a persistent variant known as chronic intestinal pseudo-obstruction (CIP).
Causes
Typically, the coordinated action of nerves and muscles generates rhythmic contractions facilitating the movement of food through the intestines. However, in cases of intestinal pseudo-obstruction, abnormalities in either nerves or muscles disrupt these contractions. Consequently, individuals with this condition experience difficulties in the passage of food, fluid, and air through the intestines.
When the underlying cause of the nerve or muscle issues triggering intestinal pseudo-obstruction is unidentified, it is termed primary or idiopathic intestinal pseudo-obstruction. Alternatively, if the cause is known, the condition is referred to as secondary intestinal pseudo-obstruction. Factors leading to secondary intestinal pseudo-obstruction include:
- Abdominal or pelvic surgery
- Diseases affecting muscles and nerves, such as lupus erythematosus, scleroderma, and Parkinson’s disease
- Infections
- Medications, such as opiates and antidepressants, that impact muscles and nerves
Symptoms
Symptoms of intestinal pseudo-obstruction can manifest as cramps, abdominal pain, nausea, vomiting, bloating, and constipation. In certain cases, diarrhea may also occur. Gradually, this condition can lead to bacterial infections, malnutrition, weight loss, and muscle issues in various body areas. Additionally, individuals may experience complications in their esophagus, stomach, or bladder.
Diagnosis
Treatment
Individuals with intestinal pseudo-obstruction often require nutritional assistance to avert malnutrition and weight loss. Enteral nutrition involves delivering liquid food through a feeding tube inserted either through the nose into the stomach or directly into the stomach or small intestine. For some, intravenous feeding, known as parenteral nutrition, is necessary, administering liquid food through a tube placed in a vein.
If intestinal pseudo-obstruction stems from an underlying illness or medication, the doctor will address the root cause by treating the illness or discontinuing the medication.
Treatment approaches may encompass medications like antibiotics for bacterial infections, pain relievers, and drugs targeting intestinal muscle issues. Individuals with acute colonic pseudo-obstruction (ACPO) may undergo procedures to alleviate gas from the bowel. In severe cases of intestinal pseudo-obstruction, surgical interventions, such as removing a portion of the intestine or other intestinal procedures, may be imperative.
Key points to bear in mind:
- Intestinal pseudo-obstruction mirrors symptoms of bowel obstruction, but upon examination, no physical blockage is detected.
- The condition arises from nerve or muscle complications hindering normal intestinal contractions necessary for propelling food, fluid, and air through the intestines.
- Symptoms encompass cramps, abdominal pain, nausea, vomiting, bloating, constipation, and occasionally diarrhea.
- Treatment varies based on the type and severity of intestinal pseudo-obstruction, potentially involving nutritional support, medications, surgery, or other procedural interventions.
References
The National Digestive Diseases Information Clearinghouse (NDDIC)
National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
