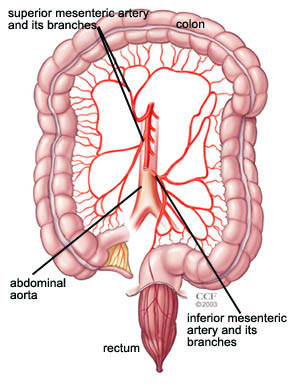
Intestinal Ischemia:
Intestinal ischemia refers to a condition in which blood flow to the intestines is reduced or blocked, leading to insufficient oxygen and nutrients reaching the intestinal tissues. This reduction in blood supply can result in damage to the intestines and, if left untreated, can lead to serious complications.
There are two main types of intestinal ischemia:
Acute Mesenteric Ischemia (AMI): This is a sudden and severe decrease in blood flow to the intestines. It is often caused by a blood clot that blocks one of the arteries supplying the intestines. Other potential causes include emboli (blood clots that travel from other parts of the body) or conditions that cause the blood vessels to narrow.
Chronic Mesenteric Ischemia (CMI): This is a gradual and long-term decrease in blood flow to the intestines. It is usually caused by atherosclerosis, a condition where fatty deposits (plaque) build up in the arteries, narrowing them over time.
Symptoms of intestinal ischemia may include severe abdominal pain, nausea, vomiting, and diarrhea. If left untreated, it can lead to tissue damage, infection, and, in severe cases, gangrene. Diagnosis typically involves imaging studies such as CT scans or angiography to visualize blood flow in the intestines. Treatment may involve addressing the underlying cause, surgery to remove clots or repair blood vessels, and supportive measures to manage symptoms. Intestinal ischemia is a serious condition that requires prompt medical attention. If you suspect you or someone else may be experiencing symptoms, it is crucial to seek immediate medical care.
Causes
Intestinal ischemia and infarction can arise from various factors. These include:
- Hernia: When the intestine displaces or becomes entangled, it can result in intestinal ischemia.
- Adhesions: Scar tissue from previous surgeries can trap the intestine (adhesions), potentially leading to ischemia if not addressed.
- Embolus: A blood clot originating from the heart or major blood vessels may travel through the bloodstream, obstructing arteries that supply the intestine. Individuals with prior heart attacks or arrhythmias, such as atrial fibrillation, are susceptible to this issue.
- Arterial thrombosis: Atherosclerotic disease (cholesterol buildup) may narrow the arteries supplying blood to the intestine, causing blockage. Similar to a heart attack in coronary arteries, arterial thrombosis results in intestinal ischemia.
- Venous thrombosis: Blood clots may block the veins responsible for carrying blood away from the intestines, impeding blood flow into the intestines. This is more prevalent in individuals with liver disease, cancer, or blood clotting disorders.
- Low blood pressure: Severe hypotension in patients with pre-existing narrowing of intestinal arteries can induce intestinal ischemia. This typically occurs in critically ill patients, akin to reduced water pressure in a hose with partial blockage.
Symptoms
The hallmark of intestinal ischemia is abdominal pain. Other symptoms include:
- Diarrhea
- Fever
- Vomiting
Diagnosis
Treatment, Complications, and Outcome
Treatment typically involves surgical intervention. The affected portion of the intestine, which has experienced necrosis, is excised, and the remaining healthy ends of the bowel are then reconnected. In certain instances, a colostomy or ileostomy may be necessary. If there is a blockage in the arteries supplying the intestine, efforts are made to correct it. Cases of intestinal infarction may necessitate either a temporary or permanent colostomy or ileostomy, and peritonitis is a common occurrence in such situations. The severity of the illness can lead to fever and bloodstream infection (sepsis). Intestinal ischemia is a grave condition that can prove fatal if not promptly addressed. The prognosis depends on the underlying cause, and a positive outcome can be achieved with swift and timely treatment.
References
Fry RD, Mahmoud N, Maron DJ, Ross HM, Rombeau J. Colon and rectum. In: Townsend CM Jr, Beauchamp RD, Evers MB, Mattox KL, eds. Sabiston Textbook of Surgery. 18th ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 50.
Hauser SC. Vascular diseases of the gastrointestinal tract. In: Goldman L, Ausiello D, eds. Cecil Medicine. 23rd ed. Philadelphia, Pa: Saunders Elsevier; 2007:chap 146.
Updated by: David C. Dugdale, III, MD, Professor of Medicine, Division of General Medicine, Department of Medicine, University of Washington School of Medicine; and George F. Longstreth, MD, Department of Gastroenterology, Kaiser Permanente Medical Care Program, San Diego, California. Also reviewed by David Zieve, MD, MHA, Medical Director, A.D.A.M., Inc.
