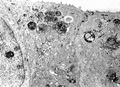
Microvillous Inclusion Disease:
Microvillous Inclusion Disease, also referred to as Davidson’s disease, congenital microvillous atrophy, or more broadly as microvillous atrophy, is a rare genetic disorder affecting the small intestine. It follows an autosomal recessive inheritance pattern. The condition manifests as persistent and difficult-to-treat diarrhea in newborns, typically emerging within the initial days of life. This leads to metabolic acidosis and profound dehydration. It’s noteworthy that pregnancy and childbirth experiences are generally unremarkable in individuals with this condition.
Diagnosis
Diagnosis in utero is currently not possible as the gene(s) involved in the disease was only recently discovered. Diagnosis is made by biopsy of the small intestine.[1]
Biopsy
The appearance of microvillous inclusion disease on light microscopy is similar to celiac sprue; however, it usually lacks the intraepithelial lymphocytic infiltration characteristic of celiac sprue and stains positive for carcinoembryonic antigen (CEA).[2] The definitive diagnosis is dependent on electron microscopy.[6]
Differential diagnosis
The possible causes for chronic and intractable diarrhea include:
- Intestinal epithelial dysplasia
- Syndromatic diarrhea
- Immunoinflammatory enteropathy
Note: The information provided is based on the given text, and it’s important to consult with a healthcare professional for accurate diagnosis and guidance.
Genetics & Prevalence
Microvillous inclusion disease is considered extremely rare, with only about two dozen cases reported in the medical literature.[8] In Arizona, a teenage girl started developing microvilli after thirteen years of dependence on Total Parenteral Nutrition (TPN) and Lipids. She has since transitioned to a typical teenage diet and receives regular care from her Gastroenterologist.
In the UK, a documented case noted a patient achieving nutritional independence at the age of 3.[9]
Meanwhile, in the Netherlands, another patient relied on enteral nutrition instead of parenteral nutrition, without exhibiting any MYO5B mutations.[5]
Tragically, on June 26, 2009, a six-year-old girl diagnosed with microvillous inclusion disease became the third person in the UK to succumb to swine flu.[10]
Treatment
Historically, various medications have been experimented with to halt or mitigate severe diarrhea in cases of microvillus inclusion disease, but none have demonstrated effectiveness. Infants with this condition depend on intravenous administration of nutritionally balanced formulas, a method known as total parenteral nutrition (TPN), to ensure adequate nourishment. While TPN can temporarily stabilize a baby’s health, it is not an ideal long-term solution. Prolonged use of TPN may lead to liver damage and elevate the susceptibility to infections. In instances where TPN gives rise to such complications, intestinal transplantation frequently emerges as the preferred alternative.
References
- ^ a b Chehade, Mirna; Sicherer, Scott H (2005). “Infantile food protein-induced enterocolitis syndrome”. In David, Timothy J. Recent Advances in Paediatrics 22. London: Royal Society of Medicine Press. pp. 140. ISBN 1853155721
- ^ a b Mills SE, Carter D, Greenson JK, Oberman HA, Reuter V, Stoler MH. Sternberg’s Diagnostic Surgical Pathology. 4th Ed. Lippincott Williams & Wilkins. Copyright 2004. ISBN 978-0-7817-4051-7.
- ^ a b Salvatore, S.; Hauser, B.; Vandenplas, Y. (2007). “Chronic enteropathy and feeding”. In Cooke, Richard J.; Vandenplas, Yvan; Wahn, Ulrich. Nutrition Support for Infants and Children at Risk. Basel, Switzerland; New York: Karger. pp. 123. ISBN 3805581947
- ^ Arpin, M.; Crepaldi, T.; Louvard, D. (1999). “Cross-talk between Apical and Basolateral Domains of Epithelial Cells Regulates Microvillus Assembly”. In Birchmeier, Walter; Birchmeier, Carmen. Epithelial Morphogenesis in Development and Disease. Amsterdam: Harwood Academic. pp. 104. ISBN 9057024195
- ^ a b Mueller T; Hess, MW; Schiefermeier, N; Pfaller, K; Ebner, HL; Heinz-Erian, P; Ponstingl, H; Partsch, J et al. (2008). “MYO5B mutations cause microvillus inclusion disease and disrupt epithelial cell polarity”. Nat Genet 40 (10): 1163–5. doi:10.1038/ng.225. PMID 18724368.
- ^ Kennea N, Norbury R, Anderson G, Tekay A (2001). “Congenital microvillous inclusion disease presenting as antenatal bowel obstruction”. Ultrasound Obstet Gynecol 17 (2): 172–4. doi:10.1046/j.1469-0705.2001.00211.x. PMID 11251929.
- ^ Ruemmele FM (2007). “Chronic enteropathy: molecular basis”. Nestle Nutr Workshop Ser Pediatr Program 59: 73–85; discussion 85–8. doi:10.1159/000098514.PMID 17245092.
- ^ Online ‘Mendelian Inheritance in Man’ (OMIM) Microvillous atrophy -251850
- ^ Croft NM; Howatson, AG; Ling, SC; Nairn, L; Evans, TJ; Weaver, LT (2000). “Microvillous inclusion disease: An evolving Condition”. J Pediatr Gastroenterol Nutr 32 (2): 185–189.PMID 10941974.
- ^ “Swine flu girl ‘had tough life'”. BBC News. 30 June 2009. Retrieved 12 May 2010.
- ^ Davidson GP, Cutz E, Hamilton JR, Gall DG (1978). “Familial enteropathy: a syndrome of protracted diarrhea from birth, failure to thrive, and hypoplastic villus atrophy”.Gastroenterology 75 (5): 783–90. PMID 100367.
