Jejunoileal Atresia:
Jejunoileal atresias represent total blockages occurring either in the jejunum or ileum of the gastrointestinal tract. These obstructions arise due to abnormalities in both arterial and venous structures within the mesentery of the developing fetus’s bowel. While this condition is more frequently observed in the jejunum, it occurs with equal prevalence in both males and females. Additionally, jejunoileal atresias can manifest as either singular or multiple obstructions, further contributing to the complexity of the condition. In comparison to duodenal atresias, jejunoileal atresias are associated with fewer anomalies. This distinction underscores the unique nature of jejunoileal atresias and emphasizes the varied presentations and characteristics within the spectrum of gastrointestinal obstructions.
Classification
Jejunoileal atresia is a condition characterized by an obstruction in the middle region (jejunum) or lower region (ileum) of the small intestine. The affected part of the intestine undergoes expansion, diminishing its capacity to absorb nutrients and propel its contents through the digestive tract. There are four subtypes of jejunoileal atresia:
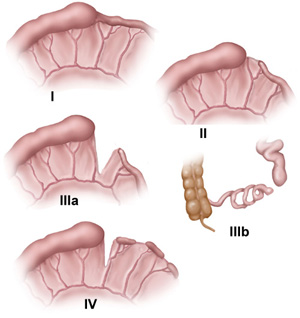
- Intestinal Atresia Type I: Involves the formation of a web-like membrane inside the intestine during fetal development, blocking the passage. However, the intestine typically develops to a normal length.
- Intestinal Atresia Type II: Features a dilated section of the intestine forming a blind end, connected to a smaller segment by scar tissue. The intestine develops to a normal length.
- Intestinal Atresia Type III: Two blind ends of the intestine are separated by a flaw in the intestinal blood supply, significantly reducing its length. This may lead to long-term nutritional deficiencies or short gut syndrome.
- Intestinal Atresia Type IV: Involves multiple blocked sections of the intestine, resulting in a very short length of functional intestine.
Infants with any of these subtypes typically exhibit green bile vomiting within a day of birth. However, those with obstructions farther down the intestine may not experience vomiting until two to three days later. Additionally, a baby with jejunoileal atresia may present with a swollen belly and may not have a bowel movement during the first day of life, unlike most infants.
Diagnosis
Prenatal ultrasounds are increasingly detecting intestinal obstructions, signaled by indicators such as excess amniotic fluid (polyhydramnios) resulting from the inadequate absorption of amniotic fluid by the intestine. When there’s suspicion of intestinal atresia or stenosis, the following diagnostic procedures are typically conducted after stabilizing the infant:
- Abdominal X-ray: Often sufficient for diagnosis in most cases.
- Lower Gastrointestinal (GI) Series: This procedure examines the rectum, large intestine, and lower part of the small intestine using an X-ray contrast agent administered as an enema. It reveals narrowed areas, obstructions, bowel width (caliber), and other issues.
- Upper GI Series: Focusing on the upper digestive system, particularly beneficial for cases involving upper intestinal obstruction (pyloric or duodenal atresia). Barium, a liquid visible on X-rays, is either ingested or introduced through a tube to assess digestive organs via X-rays.
- Abdominal Ultrasound: Utilizing ultrasonography to observe internal organs in action and assess blood flow. Gel is applied to the abdomen, and a transducer sends sound waves into the body, producing images on a monitor. The test can be recorded for later review.
In cases of intestinal atresia with associated life-threatening abnormalities, echocardiography and additional imaging studies of the cardiac and renal regions may also be conducted post-stabilization of the infant.
Treatment
Jejunoileal atresia surgery is tailored to the specific type of atresia, the extent of the intestinal involvement, and the degree of dilation. The most common procedure involves excising the non-functional intestinal segments, and the remaining ends are closed using sutures. In cases of a narrowed (stenosed) intestinal segment, surgical intervention may entail its removal, followed by suturing the bowel to restore intestinal continuity.
The surgical procedure is conducted under general anesthesia with meticulous monitoring in a heated operating room. The nature of the defect dictates the surgical approach:
Type I:
- An incision is made in the bowel wall at the web level, the web is removed, and the bowel wall is sutured (jejunoplasty).
- Alternatively, the abnormal bowel may be resected, and the cut ends are anastomosed (sewn together).
Type II – IV:
- The atretic bowel segment is removed, and anastomosis is performed to suture the cut ends together.
Outcomes
Infants diagnosed with intestinal atresia undergo management using a nasogastric tube, which remains in place until their bowel function returns, a process that can span from a few days to several weeks. During the period of bowel inactivity, nutrition is administered intravenously. Once normal intestinal function is restored, nutrition is transitioned to oral intake or delivered through a feeding tube.
Regarding the long-term outlook for children who have undergone surgery for intestinal atresia, regular follow-up is essential to monitor growth, development, and prevent potential nutritional deficiencies resulting from the loss of intestine.
The progression of infants largely depends on the presence of associated abnormalities and the remaining length of the intestine. Generally, most infants recover well, with rare complications post-surgery. In the immediate to early postoperative period, there may be a risk of intestinal contents leaking at the suture line, potentially leading to abdominal infections requiring additional surgery. Later complications may include malabsorption syndromes, functional obstruction due to an enlarged and paralyzed segment of the intestine, or the development of short gut syndrome.
References
Cincinnati Children’s Hospital Medical Center
http://www.cincinnatichildrens.org/health/i/obstructions/
YourSurgery.Com
http://yoursurgery.com/ProcedureDetails.cfm?BR=1&Proc=77
-Jejunoileal Atresia
