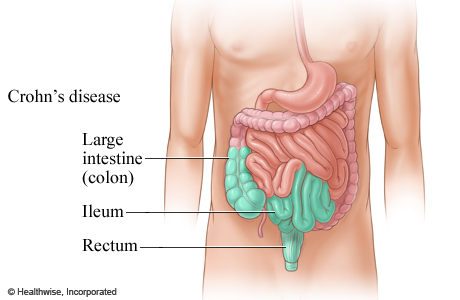
🩺 Crohn’s Disease: Symptoms, Types, & Management
Crohn’s disease is a chronic, inflammatory bowel disease (IBD) characterized by systemic, transmural inflammation that can affect any part of the digestive tract, from the mouth to the anus.
Unlike other inflammatory conditions, Crohn’s disease can present with “skip lesions”—areas of severe inflammation interspersed with patches of completely healthy tissue. Because it damages the intestinal lining across multiple sections, it stands as one of the leading causes of Short Bowel Syndrome.
🔬 5 Types of Crohn’s Disease
The condition is categorized based on the specific region of the gastrointestinal (GI) tract it targets:
1. Gastroduodenal Crohn’s Disease
-
Location: Impacts the stomach and the duodenum (the first part of the small intestine).
-
Key Features: Frequently misdiagnosed as peptic ulcer disease. True diagnosis often occurs only after ulcer treatments fail.
-
Symptoms: Loss of appetite, weight loss, nausea, upper-middle abdominal pain, and vomiting.
2. Jejunoileitis
-
Location: Affects the jejunum (the midsection of the small intestine).
-
Key Features: High risk of nutrient malabsorption leading to malnutrition. It frequently causes fistulas (abnormal tunnels linking the diseased bowel to other organs or loops of intestine).
-
Symptoms: Severe abdominal cramps after eating, diarrhea, and nutrient deficiencies.
3. Ileitis
-
Location: Targets the ileum (the final segment of the small intestine).
-
Key Features: Can cause inflammatory masses or fistulas. Damage to the ileum impairs Vitamin $\text{B}_{12}$ and folate absorption, which can trigger peripheral neuropathy and macrocytic anemia.
-
Symptoms: Diarrhea, cramping, and sharp pain localized to the lower right quadrant.
4. Ileocolitis
-
Location: Affects both the ileum and the colon simultaneously.
-
Key Features: The most prevalent form of Crohn’s disease. It typically concentrates around the ileocecal valve.
-
Symptoms: Severe diarrhea, cramping, right lower quadrant pain, and significant weight loss.
5. Crohn’s Colitis (Granulomatous Colitis)
-
Location: Confined strictly to the large intestine (colon).
-
Key Features: Differentiated from Ulcerative Colitis (UC) because it leaves patches of healthy tissue between inflamed zones and frequently spares the rectum entirely (UC is always continuous and always involves the rectum).
📋 Signs & Symptoms
The clinical features of Crohn’s disease are split between gastrointestinal distress and systemic, extraintestinal manifestations.
Gastrointestinal Symptoms
-
Diarrhea: Frequent, loose, or watery stools. They may contain dark, thick blood (melena) if inflammation is extreme, though they characteristically contain less mucus or pus than Ulcerative Colitis.
-
Abdominal Pain: Varies by location. Disease in the terminal ileum causes sharp pain in the lower right quadrant and periumbilical area, which often intensifies after meals and temporarily eases after a bowel movement. Colonic disease causes generalized, crampy pain.
-
Fever & Night Sweats: Driven by the systemic inflammatory process. Patients may suffer from acute spikes or persistent low-grade fevers that break during sleep, causing heavy night sweats, fatigue, and irritability.
👁️ Extraintestinal Symptoms (Beyond the GI Tract)
Systemic immune responses can cause flare-ups in other systems, sometimes preceding intestinal issues by weeks or months:
-
Eyes: Redness, pain, and inflammation (iritis/uveitis).
-
Joints: Migrating arthralgia—joint pain that moves between larger joints like the knees, ankles, elbows, and wrists.
-
Skin: Erythema nodosum (tender, painful red nodules typically appearing on the shins or calves) and aphthous ulcers (painful mouth sores).
🔍 Causes & Risk Factors
Crohn’s disease is classified as idiopathic (its exact triggering cause remains unknown), involving an unregulated, overactive immune response in the gut wall.
-
Genetics: Tends to run in families. Approximately 20% to 25% of Crohn’s patients have a close relative with IBD.
-
Demographics & Ethnicity: Higher rates of incidence are observed in Western, industrialized societies and within certain ethnic groups. For instance, data indicates that in the United States, Caucasian and Jewish populations historically experience higher rates of the disease, though incidence rates have been steadily rising globally across all racial and ethnic demographics.
-
Environment: Dietary habits, industrial pollution, and altered gut microbiomes in Western societies are heavily studied as environmental triggers for initial episodes or relapses.
🩺 Diagnostic Approach
A definitive diagnosis relies on combining laboratory evaluations with direct visualization of the bowel wall:
-
Laboratory Testing: Complete blood counts (to assess for anemia and elevated white blood cells) and stool cultures (to rule out infectious colitis).
-
Imaging & Endoscopy: Direct visual examination via Colonoscopy or Sigmoidoscopy allows physicians to evaluate tissue integrity and take biopsies. A Barium Enema (X-ray with contrast dye) may be used to map structural narrowings, strictures, or fistulas.
💊 Treatment & Remission Management
There is no permanent cure for Crohn’s disease; therapeutic management focuses on checking acute inflammation, inducing clinical remission, and maintaining that remission indefinitely.
Pharmacological Therapy
-
5-ASA Compounds: Anti-inflammatory medications utilized to treat mild-to-moderate disease.
-
Corticosteroids: Powerful, fast-acting immune suppressors used short-term to halt severe, acute flare-ups (not intended for long-term maintenance due to systemic side effects).
-
Immunomodulators: Medications that quiet down the body’s overactive immune system over the long term.
-
Biologics (e.g., Infliximab / Remicade): Targeted therapies that block specific inflammatory proteins (like TNF-alpha) to promote deep mucosal healing.
-
Antibiotics: Used to manage bacterial overgrowth or treat complications like abscesses and perianal fistulas.
