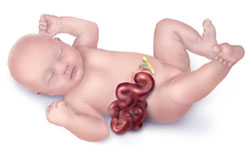
Gastroschisis:
Gastroschisis is a congenital anomaly characterized by a structural defect in the anterior abdominal wall, allowing the intestinal contents to protrude freely outside the baby’s body. This condition typically manifests as the baby’s intestines extending through a hole located beside the belly button. In addition to the intestines, other organs such as the stomach and liver may also protrude beyond the confines of the abdominal cavity.
It is crucial to distinguish Gastroschisis from Omphalocele, as in the former, the exposed intestines lack the protective covering of a sac. This absence of a protective sac exposes the intestines to the amniotic fluid surrounding the baby in the womb. Consequently, the bowel may be subjected to irritation, leading to potential complications such as shortening, twisting, or swelling.
The absence of a sac in Gastroschisis poses unique challenges, as the exposed intestines are more susceptible to the effects of the amniotic fluid. This exposure can result in complications that may affect the normal development and function of the bowel. It is important for medical professionals to closely monitor and manage cases of Gastroschisis to mitigate potential risks and ensure the best possible outcome for the newborn.
Causes
Complications in pregnancies, particularly those involving infection, young maternal age, smoking, drug abuse, or factors leading to low birth weight, may elevate the risk of gastroschisis. This condition is more prevalent in newborns with intrauterine growth retardation, contributing to small gestational age. The relationship between intrauterine growth retardation facilitating gastroschisis or the abdominal wall defect hindering fetal growth remains unclear.
Recent research suggests a potential link between a change in paternity (childbearing with different fathers) and an increased risk of gastroschisis, hinting at the involvement of the mother’s immune system in its development.
Gastroschisis, when occurring as an isolated congenital defect, typically follows an autosomal recessive inheritance pattern. While it may start as a sporadic mutation, it can also be associated with non-genetic congenital disorders or manifest as autosomal dominant.
Considering the genetic implications, genetic counseling and additional testing, such as amniocentesis, may be offered during pregnancy, especially since abdominal wall defects like gastroschisis are linked to genetic disorders. If there are no accompanying genetic problems or birth defects, early surgical intervention post-birth can often successfully repair the opening.
An In-Depth Look
At least six hypotheses have been proposed:
- Failure of mesoderm to form in the body wall[4]
- Rupture of the amnion around the umbilical ring with subsequent herniation of bowel[5]
- Abnormal involution of the right umbilical vein leading to weakening of the body wall and gut herniation[6]
- Disruption of the right vitelline (yolk sac) artery with subsequent body wall damage and gut herniation[7]
- Abnormal folding of the body wall results in a ventral body wall defect through which the gut herniates[8]
- Failure to incorporate the yolk sac and related vitelline structures into the yolk sac[9]
The first hypothesis does not explain why the mesoderm defect would occur in such a specific small area. The second hypothesis does not explain the low percentage of associated abnormality compared with omphalocele. The third hypothesis was criticized due to no vascular supplement of anterior abdominal wall by umbilical vein. The fourth hypothesis was commonly accepted, but it was later shown that the right vitelline artery (right omphalomesenteric artery) did not supply the anterior abdominal wall in this area.[10]More evidence is needed to support the fifth hypothesis.[8]
Complications in pregnancies, particularly those involving factors such as infection, young maternal age, smoking, and drug abuse, as well as conditions leading to low birth weight, may contribute to an elevated risk of gastroschisis. This congenital anomaly is more prevalent in newborns with intrauterine growth retardation, a condition that contributes to small gestational age. The intricate relationship between intrauterine growth retardation facilitating the development of gastroschisis or the abdominal wall defect hindering fetal growth remains ambiguous.
Recent research has introduced a novel perspective, suggesting a potential link between a change in paternity, specifically childbearing with different fathers, and an increased risk of gastroschisis. This intriguing finding hints at the possible involvement of the mother’s immune system in the development of this condition.
Gastroschisis, when it occurs as an isolated congenital defect, typically follows an autosomal recessive inheritance pattern. While it may originate as a sporadic mutation, it can also be associated with non-genetic congenital disorders or manifest as autosomal dominant. Understanding the genetic implications becomes crucial, prompting the consideration of genetic counseling and additional testing, such as amniocentesis, during pregnancy. This is particularly relevant since abdominal wall defects, like gastroschisis, are often linked to genetic disorders.
In cases where there are no accompanying genetic problems or birth defects, early surgical intervention post-birth can often lead to successful repair of the abdominal opening. The comprehensive approach, encompassing both genetic assessment and timely medical intervention, underscores the multidimensional nature of managing pregnancies at risk for gastroschisis.
Risks & Outcomes
Recently, researchers from the Centers for Disease Control and Prevention (CDC) have unveiled significant findings regarding factors influencing the risk of gastroschisis in newborns:
- Age: Teenage mothers exhibit a higher likelihood of having a baby with gastroschisis compared to older mothers. Among teenagers, White individuals have higher rates than Black or African-American counterparts.
- Alcohol and Tobacco: Women who consume alcohol or are smokers are at an increased risk of giving birth to a baby with gastroschisis.
- Medications: The use of ibuprofen during pregnancy has been identified as a factor that raises the risk of gastroschisis.
- Infections: Women reporting genitourinary tract infections just before or during early pregnancy face an elevated risk of having a baby with gastroschisis.
The CDC is actively researching birth defects like gastroschisis to enhance understanding and develop preventive measures. If you are pregnant or planning to conceive, it is advisable to consult your doctor regarding strategies to increase the likelihood of a healthy baby.
Following birth, surgery becomes necessary to reposition the abdominal organs inside the baby’s body and address the gastroschisis defect.
For smaller gastroschisis defects (where only a portion of the intestine is outside the belly), surgery is typically performed shortly after birth to return the organs to the belly and close the opening. In cases of larger defects (involving multiple organs outside the belly), the repair may be conducted gradually, in stages. Special materials may be used to cover exposed organs, slowly relocating them back into the belly. Once all organs are returned, the opening is closed.
Babies with gastroschisis often require additional treatments, including receiving nutrients through an IV line, antibiotics to prevent infection, and meticulous attention to maintaining their body temperature.
References
- ^ Schwartz’s principles of surgery: self assessment and board review, 8th edition, chapter 38, page 278; textbook p.1493
- ^ Chambers, Christina D.; Chen, Brian H.; Kalla, Kristin; Jernigan, Laura; Jones, Kenneth Lyons (2007). “Novel risk factor in gastroschisis: Change of paternity”.American Journal of Medical Genetics Part A 143A (7): 653–659.doi:10.1002/ajmg.a.31577. PMID 17163540.
- ^ Yang, Ping; Beaty, Terri H.; Khoury, Muin J.; Chee, Elsbeth; Stewart, Walter; Gordis, Leon (1992). “Genetic-epidemiologic study of omphalocele and gastroschisis: Evidence for heterogeneity”. American Journal of Medical Genetics 44 (5): 668–675.doi:10.1002/ajmg.1320440528. PMID 1481831.
- ^ Duhamel, B. (1963). “Embryology of Exomphalos and Allied Malformations”.Archives of Disease in Childhood 38: 142–7. doi:10.1136/adc.38.198.142.
- ^ Shaw, Anthony (1975). “The myth of gastroschisis”. Journal of Pediatric Surgery 10(2): 235–44. doi:10.1016/0022-3468(75)90285-7. PMID 123582.
- ^ Devries, Pieter A. (1980). “The pathogenesis of gastroschisis and omphalocele”.Journal of Pediatric Surgery 15 (3): 245–51. doi:10.1016/S0022-3468(80)80130-8.PMID 6445962.
- ^ Hoyme, H; Higginbottom, M; Jones, K (1981). “The vascular pathogenesis of gastroschisis: Intrauterine interruption of the omphalomesenteric artery”. The Journal of Pediatrics 98 (2): 228–31. doi:10.1016/S0022-3476(81)80640-3.PMID 6450826.
- ^ a b c Feldkamp, Marcia L.; Carey, John C.; Sadler, Thomas W. (2007). “Development of gastroschisis: Review of hypotheses, a novel hypothesis, and implications for research”. American Journal of Medical Genetics Part A 143A: 639–52.doi:10.1002/ajmg.a.31578.
- ^ Stevenson, RE; Rogers, RC; Chandler, JC; Gauderer, MWL; Hunter, AGW (2009). “Escape of the yolk sac: a hypothesis to explain the embryogenesis of gastroschisis”.Clinical Genetics 75 (4): 326–33. doi:10.1111/j.1399-0004.2008.01142.x.PMID 19419415.
- ^ Curry, Cynthia; Boyd, Ellen; Stevenson, Roger E. (2006). “Ventral Wall of the Trunk”. In Stevenson, Roger E.; Hall, Judith G.. Human Malformations and Related Anomalies. Oxford: Oxford University Press. pp. 1023–49. ISBN 978-0-19-516568-5.
